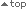*In patients with CCyR.
Ranges are in parentheses.
CCyR, complete cytogenetic response; IQ, interquartiles; MMR, major molecular response.
- European Treatment and Outcome Study
- Registry
- Molecular Monitoring
- Path to cure
- Spread of Excellence
Case-Based Review
Table of contents
Editorial Reviewers: Merrill J. Egorin, MD, FACP; François-Xavier Mahon, MD, PhD
You can get the PDF-brochure, here
Background
Chronic myeloid leukemia (CML) is a proliferative disease characterized in 95% of patients by the presence of the Philadelphia chromosome, which is generated by a reciprocal t(9;22) chromosome translocation in a hematopoietic stem cell.1,2 This aberrant chromosome harbors a BCR-ABL fusion gene that encodes BCR-ABL, a fusion protein with deregulated (constitutive) tyrosine kinase activity that contributes to malignant transformation. BCR-ABL tyrosine kinase activity results in excessive proliferation and decreased apoptosis of CML cells, as well as decreased sensitivity to the regulatory influence of bone marrow stromal cells, leading to massive clonal expansion.3,4
Identification of the underlying cause of CML led to the development of rationally designed drugs that target BCR-ABL tyrosine kinase activity as potential treatment for this disease. One of these drugs, Glivec®/Gleevec® (imatinib mesylate; STI571), is a 2-phenylaminopyrimidine that inhibits the tyrosine kinase activity of BCR-ABL, as well as certain other protein tyrosine kinases.5-8 More effective than previous therapies for CML, Imatinib is now the standard of care for this disease.9,10
Imatinib has activity in all phases of CML but produces its most extensive and durable responses in newly diagnosed patients with chronic-phase disease. Analysis of follow-up data for patients with newly diagnosed CML who received Glivec/Gleevec as initial therapy in the International Randomized Interferon Versus STI571 (IRIS) study 11,12 showed that, at 60 months after initiation of therapy, 89% of the patients were still alive.13 This rate is higher than that reported in any previously published prospective study of CML treatment. Moreover, by 60 months, 87% of patients had achieved a complete cytogenetic response (CCyR). Glivec/Gleevec also induces therapeutic responses in patients with advanced (accelerated phase or blast crisis) CML; however, response rates are lower, and relapse commonly occurs within 1 year.14-16
Relapse or suboptimal response in patients receiving Imatinib therapy can be caused by several factors, including emergence of point mutations within the gene encoding the kinase domain of the BCR-ABL protein that reduce the binding affinity of Imatinib, amplification
of the BCR-ABL gene and overexpression of the multidrug resistance (MDR) gene encoding
P-glycoprotein.17,18 However, pharmacokinetic variability and nonadherence to the prescribed Imatinib dosage regimen may also play a role in variable responses to Imatinib.19-21
Pharmacokinetic Factors and Response to Imatinib
Many factors alter the disposition of Glivec/Gleevec: decreased absorption due to gastrointestinal anatomic abnormalities or disease states that interfere with this process; binding to plasma proteins, mainly alpha 1 acid-glycoprotein and albumin; interaction with drugs that increase or decrease the activity of major metabolic enzymes of Imatinib such as CYP3A4; and extrusion by efflux transporters such as P-glycoprotein. These factors can affect the plasma concentration (level) of Imatinib over time and subsequently alter its pharmacologic effect.20,22-27 Evidence suggests that plasma concentrations of Imatinib correlate with clinical response,28,29 and thus too low a plasma concentration of this agent can result in decreased efficacy, seen as failure to achieve or maintain a CCyR or a major molecular response (MMR).
A correlation was found in a phase 1 study between hematologic response and Imatinib dose, area under the time/concentration curve (AUC), maximum plasma concentration (Cmax), and trough plasma concentration (Cmin).19 A correlation between Imatinib Cmin
and achievement of a CCyR or MMR with standard-dose Imatinib in patients with chronic-phase (CP) or accelerated-phase (AP) CML (CML-CP or CML-AP) was found in another study.29 Samples for determination of Imatinib trough plasma concentrations were obtained approximately 24 hours after the last dose in 68 patients. The analysis showed that, after 12 months of treatment, mean trough plasma concentrations of Imatinib were significantly higher in patients who achieved CCyR or MMR compared with patients who did not reach these levels of response (CCyR: 1.123 ± 0.617 µg/mL vs 0.694 ± 0.556 µg/mL, P = 0.03; MMR: 1.452 ± 0.649 µg/mL vs 0.869 ± 0.427 µg/mL; P < 0.0001). In the IRIS study, the relationship between clinical response and steady-state trough plasma concentrations of Imatinib after 400-mg dosing was examined in newly diagnosed patients with CML-CP.28 Trough plasma concentrations were measured at day 1 and day 29 (steady state), and patients were then stratified according to drug trough concentration (lower quartile [Q1], values in the range of 0%-<25%; interquartiles [Q2 + Q3], values in the range of 25%-75%; upper quartile [Q4], values in the range of >75%-100%). Day 29 trough plasma concentrations of Imatinib were predictive of CCyR or MMR at both 1 year and 4 years. The Cmin of Imatinib was significantly higher in patients who achieved CCyR compared with patients who did not (1.01 µg/mL vs 0.812 µg/mL [P = 0.0116]). Rates of MMR at 1 year were lower in patients in the lowest Imatinib plasma concentration quartile compared with all other patients (25% vs 40%) (Figure 1).28
Trough plasma concentrations following the first dose of Imatinib also correlated with CCyR and MMR rates, but were less predictive than the steady-state trough level. Together, results of these studies suggest that monitoring to ensure adequate Imatinib trough plasma concentrations could be useful in optimizing response in patients with CML.
Figure 1: Correlation between response rates and imatinib trough levels after 1 year and 4 years of treatment 28

Impact of Adherence on Response to Imatinib
Adherence to (compliance with) the prescribed regimen may also influence Imatinib plasma concentration, with failure to follow the prescribed regimen potentially resulting in drug plasma concentration below the target concentration. This is a concern for physicians treating their oncology patients, as non-adherence to standard oral antineoplastic agent regimens has been associated with worsening of disease, increased physician visits and hospitalizations, unnecessary diagnostic testing, and changes in dose or regimen.30 Adherence rates for oral antineoplastics range from 20% to 100%; patients may over-estimate their adherence by a factor of 2 in discussions with their physicians.30 Typical reasons given by patients for not taking their medication as prescribed are that they forgot, had other priorities, or were experiencing unpleasant side effects. Often, patients are unaware of the critical importance of taking their medication as prescribed.
Adherence to Imatinib dosing was specifically investigated in a study that reviewed patient-level pharmacy claims data for 4043 patients with either CML or gastrointestinal stromal tumor.31 Analysis of these data revealed that, on average, CML patients took only 78%
of their prescribed medication. Moreover, all patients were on therapy for only 62% of the study period (255 days out of 24 months), with adherence beginning to decline after 4 months of treatment (Figure 2). For patients with serious medical conditions, adherence rates of 95% or greater are considered the goal.32
Factors driving suboptimal adherence and persistency can be summarized in 4 major points. The first is an inadequate response to initial doses. This can lead patients or physicians to stop or to switch treatment before considering a dose increase when indicated and giving the current medication time to reach peak plasma concentrations. Another factor is the patient misperception that a positive treatment response represents a “cure.” Such misperception can also lead to treatment drop-off, as the patient erroneously believes that he or she no longer
needs to take the medication. A third factor is patient- or physician-initiated treatment interruptions, for a variety of reasons. These can include inconvenient scheduling, forgetting to take a dose, or “taking a break” from therapy. The fourth, and arguably the most important factor contributing to suboptimal compliance, is poor side-effect management. Unaddressed side effects may cause patients to stop or lower treatment dosing on their own in an attempt to minimize the adverse reactions, or physicians will initiate the treatment interruption until side effects abate on their own.
Potential strategies to overcome problems with adherence to therapy include patient education, improved communication between physicians and patients regarding treatment expectations, improved dosing schedules for optimizing convenience, and the effective management of side effects. Therefore, clinical experts recommend routine patient support programs and improved communications to help optimize patient outcomes.
Figure 2: Adherence* to imatinib 31

*Time on therapy without significant gaps in refills.
Monitoring Imatinib Levels in CML Patients
Clearly, monitoring Imatinib plasma concentrations to ensure that the target concentration is being achieved can be a useful strategy for optimizing the benefits of Imatinib therapy. There are several situations in which you may want to consider testing Imatinib plasma levels in CML patients.
- You suspect the patient may be nonadherent to Imatinib therapy.
- You suspect the patient may be experiencing a drug-drug interaction.
- The patient is not responding to Imatinib as well as you believe he or she should.
- The patient is experiencing side effects that are unusually severe for the dose of Imatinib being taken.
Trough plasma concentrations of Imatinib are especially suitable for monitoring as they are easy to obtain and vary less over time than the plasma AUC. Titier et al 33 recently described a high-performance liquid-chromatography method coupled to electrospray-ionization tandem mass spectrometry for the quantitation of Imatinib in human plasma. The method is rapid, simple, sensitive, and suitable for routine application. 33 Other high-performance liquid-chromatography assays have also been used to determine Imatinib plasma concentrations, including those described by Bakhtiar et al 34 and Parise et al. 35 At the recommended starting dose of 400 mg/d, the mean trough plasma concentration (SD) of Imatinib at steady state is approximately 0.98 (0.53) µg/mL. At doses of 600 mg/d administered once daily and 800 mg/d administered daily as 2 divided doses (400 mg x 2), the steady-state mean trough plasma concentrations are approximately 1.37 (0.82) and 2.88 (1.09) µg/mL, respectively (Figure 3).19,36,37
The minimum effective plasma concentration of Imatinib has not been fully defined, and the relationship between Imatinib blood concentrations and outcomes remains under investigation. Nevertheless, maintaining trough concentrations at or above the average concentration at the intended dose (1 µg/mL for 400 mg/d) is recommended when tolerable. Blood concentrations below this should be avoided, and the physician should make every effort to determine the underlying cause.
Figure 3: Pharmacokinetic trough concentrations of imatinib in patients with Ph+ CML 19,36,37

Top and bottom walls of each box represent the 75th and 25th percentiles. Whiskers (error bars) above and below each box indicate the 90th and 10th percentiles, and the dots represent the 95th and 5th percentiles.
Summary
- Inadequate Imatinib exposure due to pharmacokinetic factors or nonadherence may compromise clinical outcomes in CML patients.
- Monitoring Imatinib trough plasma concentrations could help avoid low exposure in certain clinical situations.
- Monitoring Imatinib trough plasma concentrations may ensure that the target concentration is achieved and may initiate discussion of the importance of adherence and guide clinical decision making.
The following are selected case studies describing how monitoring of trough plasma concentrations of Imatinib helped physicians to identify nonadherence or suboptimal dosing and institute measures to optimize therapy. The cases reflect treating physicians’ clinical judgment, and the steps taken may not conform to current treatment algorithms.
References
- Savage DG, Antman KH. Imatinib mesylate—a new oral targeted therapy. N Engl J Med. 2002;346:683-693.
- Goldman JM, Melo JV. Chronic myeloid leukemia—advances in biology and new approaches to treatment. N Engl J Med. 2003;349:1451-1464.
- Sawyers CL. Chronic myeloid leukemia. N Engl J Med. 1999;340:1330-1340.
- O'Dwyer M. Multifaceted approach to the treatment of bcr-abl-positive leukemias. Oncologist. 2002;7(suppl 1):30-38.
- Buchdunger E, Cioffi CL, Law N, et al. Abl protein-tyrosine kinase inhibitor STI571 inhibits in vitro signal transduction mediated by c-kit and platelet-derived growth factor receptors. J Pharmacol ExpTher. 2000;295:139-145.
- Okuda K, Weisberg E, Gilliland DG, Griffin JD. ARG tyrosine kinase activity is inhibited by STI571. Blood. 2001;97:2440-2448.
- Mol CD, Dougan DR, Schneider TR, et al.Structural basis for the autoinhibition and STI-571 inhibition of c-Kit tyrosine kinase. J Biol Chem. 2004;279:31655-31663.
- Dewar AL, Cambareri AC, Zannettino AC, et al. Macrophage colony-stimulating factor receptor c-fms is a novel target of imatinib. Blood. 2005;105:3127-3132.
- Baccarani M, Saglio G, Goldman J, et al. Evolving concepts in the management of chronic myeloid leukemia. Recommendations from an expert panel on behalf of the European LeukemiaNet. Blood. 2006;108:1809-1820.
- National Comprehensive Cancer Network. NCCN Clinical Practice Guidelines in Oncology™. Chronic Myelogenous Leukemia. Version v.1. 2007. Jenkintown, Pa: National Comprehensive CancerNetwork; 2007.
- Hughes TP, Kaeda J, Branford S, et al. Frequency of major molecular responses to imatinib or interferon alfa plus cytarabine in newly diagnosed chronic myeloid leukemia. N Engl J Med. 2003;349:1423-1432.
- O'Brien SG, Guilhot F, Larson RA, et al. Imatinib compared with interferon and low-dose cytarabine for newly diagnosed chronic-phase chronic myeloid leukemia. N Engl J Med. 2003;348:994-1004.
- Druker BJ, Guilhot F, O'Brien SG, et al. Five-year follow-up of patients receiving imatinib for chronic myeloid leukemia. N Engl J Med. 2006;355:2408-2417.
- Sawyers CL, Hochhaus A, Feldman E, et al. Imatinib induces hematologic and cytogenetic responses in patients with chronic myelogenous leukemia in myeloid blast crisis: results of a phase II study. Blood. 2002;99:3530-3539.
- Talpaz M, Silver RT, Druker BJ, et al. Imatinib induces durable hematologic and cytogenetic responses in patients with accelerated phase chronic myeloid leukemia: results of a phase 2 study. Blood. 2002;99:1928-1937.
- Silver RT, Talpaz M, Sawyers CL, et al. Four years of follow-up of 1027 patients with late chronic phase (L-CP), accelerated phase (AP), or blast crisis (BC) chronic myeloid leukemia (CML) treated with imatinib in three large phase II trials [abstract]. Blood. 2004;104:11a. Abstract 23.
- Gorre ME, Mohammed M, Ellwood K, et al. Clinical resistance to STI-571 cancer therapy caused by BCR-ABL gene mutation or amplification. Science. 2001;293:876-880.
- Mahon FX, Belloc F, Lagarde V, et al. MDR1 gene overexpression confers resistance to imatinib mesylate in leukemia cell line models. Blood. 2003;101:2368-2373.
- Peng B, Hayes M, Resta D, et al. Pharmacokinetics and pharmacodynamics of imatinib in a phase I trial with chronic myeloid leukemia patients. J Clin Oncol. 2004;22:935-942.
- Peng B, Lloyd P, Schran H. Clinical pharmacokinetics of imatinib. Clin Pharmacokinet. 2005;44:879-894.
- Wilkinson GR. Drug metabolism and variability among patients in drug response. N Engl J Med. 2005;352:2211-2221.
- Gambacorti-Passerini C, Zucchetti M, Russo D, et al. Alpha1 acid glycoprotein binds to imatinib (STI571) and substantially alters its pharmacokinetics in chronic myeloid leukemia patients. Clin CancerRes. 2003;9:625-632.
- O'Brien SG, Meinhardt P, Bond E, et al. Effects of imatinib mesylate (STI571,Glivec) on the pharmacokinetics of simvastatin, a cytochrome p450 3A4 substrate, in patients with chronic myeloid leukaemia. Br J Cancer. 2003;89:1855-1859.
- Bolton AE, Peng B, Hubert M, et al. Effect of rifampicin on the pharmacokinetics of imatinib mesylate (Gleevec,STI571) in healthy subjects. Cancer Chemother Pharmacol. 2004;53:102-106.
- Dutreix C, Peng B, Mehring G, et al. Pharmacokinetic interaction between ketoconazole and imatinib mesylate (Glivec) in healthy subjects. Cancer Chemother Pharmacol. 2004;54:290-294.
- Beumer JH, Natale JJ, Lagattuta TF, Raptis A, Egorin MJ. Disposition of imatinib and its metabolite CGP74588 in a patient with chronic myelogenous leukemia and short-bowel syndrome. Pharmacotherapy. 2006;26:903-907.
- Gleevec PI. Gleevec® (imatinib mesylate) [package insert]. East Hanover, NJ: Novartis Pharmaceuticals Corporation; 2006.
- Larson RA, Druker BJ, Guilhot F, et al. on behalf of the IRIS Study Group. Correlation of pharmacokinetic data with cytogenetic and molecular response in newly diagnosed patients with chronicmyeloid leukemia in chronic phase (CML-CP) treated with imatinib—an analysis of IRIS study data [abstract]. Presented at: American Society of Hematology; December 9-12, 2006; Orlando, Fla. Abstract 429.
- Picard S, Titier K, Etienne G, et al. Trough imatinib plasma levels are associated with both cytogenetic and moleular responses to standard-dose imatinib in chronic myeloid leukemia. Blood. 2007;109:3496-3499.
- Partridge AH, Avorn J, Wang PS, Winer EP. Adherence to therapy with oral antineoplastic agents. J Natl Cancer Inst. 2002;94:652-661.
- Tsang J, Rudychev I, Pescatore SL. Prescription compliance and persistency in chronic myelogenous leukemia (CML) and gastrointestinal stromal tumor (GIST) patients (pts) on imatinib (IM). J ClinOncol. 2006;24:330s. Abstract 6119.
- Osterberg L, Blaschke T. Adherence to medication. N Engl J Med. 2005;353:487-497.
- Titier K, Picard S, Ducint D, et al. Quantification of imatinib in human plasma by high-performance liquid chromatography-tandem mass spectrometry. Ther Drug Monit. 2005;27:634-640.
- Bakhtiar R, Lohne J, Ramos L, et al. High-throughput quantification of the anti-leukemia drug STI571 (Gleevec) and its main metabolite (CGP 74588) in human plasma using liquid chromatography-tandem mass spectrometry. J Chromatogr B Analyt Technol Biomed Life Sci. 2002;768:325-340.
- Parise RA, Ramanathan RK, Hayes MJ, Egorin MJ. Liquid chromatographic-mass spectrometric assay for quantitation of imatinib and its main metabolite (CGP 74588) in plasma. J Chromatogr B Analyt Technol Biomed Life Sci. 2003;791:39-44.
- Blasdel C, Wang Y, Lagattuta T, et al. Therapeutic drug monitoring of imatinib and impact on clinical decision making [abstract]. Blood. 2006;108:290b. Abstract 4820.
- Schmidli H, Peng B, Riviere G-J, et al. Population pharmacokinetics of imatinib mesylate in patients with chronic-phase chronic myeloid leukaemia: results of a phase III Study. Br J Clin Pharmacol. 2005;60:35-44.
- Kantarjian HM, Talpaz M, O'Brien S, et al. Dose escalation of imatinib mesylate can overcome resistance to standard-dose therapy in patients with chronic myelogenous leukemia. Blood. 2003;101:473-475.
- Buchdunger E, Zimmermann J, Mett H, et al. Inhibition of the Abl protein-tyrosine kinase in vitro and in vivo by a 2-phenylaminopyrimidine derivative. Cancer Res. 1996;56:100-104.
- Druker BJ, Tamura S, Buchdunger E, et al. Effects of a selective inhibitor of the Abl tyrosine kinase on the growth of Bcr-Abl positive cells. Nat Med. 1996;2:561-566.
- Reardon DA, Egorin MJ, Quinn JA, et al. Phase II study of imatinib mesylate plus hydroxyurea in adults with recurrent glioblastoma multiforme. J Clin Oncol. 2005;23:9359-9368.
- Smith P, Bullock JM, Booker BM, et al. The influence of St. John's wort on the pharmacokinetics and protein binding of imatinib mesylate. Pharmacotherapy. 2004;24:1508-1514.
- Frye RF, Fitzgerald SM, Lagattuta TF, Hruska MW, Egorin MJ. Effect of St John's wort on imatinib mesylate pharmacokinetics. Clin Pharmacol Ther. 2004;76:323-329.
Created by: A. Hellenbrecht , generated 2008/01/03 , last changed: 2008/08/21